Trachypithecus, which at the moment accommodates 20 species divided into 4 teams, is the most speciose…
Usage of pharmaceutical contraceptive drug for controlling Eobania vermiculata snails by baits technique
The current examine centered on evaluating the consequences of oral administration of three completely different concentrations…
Reframing cognition: getting down to biological basics
The premise of this two-part theme challenge is straightforward: the cognitive sciences ought to be a…
Ecology and evolution of migration in the freshwater eels of the genus Anguilla Schrank, 1798
In a current work I reworked a fancy and built-in textual content just like the International…
Into the Chamber of Horrors: A proposal for the resolution of nomenclatural chaos in the Scaphiophryne calcarata complex (Anura: Microhylidae), with a new species-level phylogenetic hypothesis for Scaphiophryninae
The genus Scaphiophryne (Anura: Microhylidae) incorporates at the least 9 species that, collectively with their possible…
Future call for policy making to speed up interdisciplinarity between natural and social sciences and humanities in countries such as India
It clearly unknot about the truth that science is a human (society) want primarily based course…
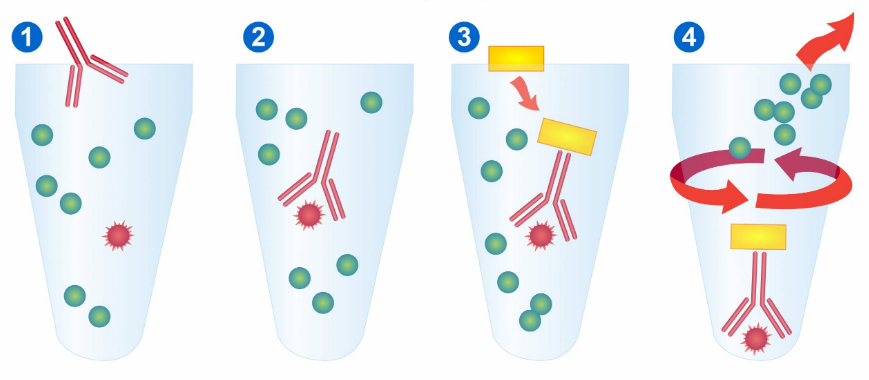
Immunoprecipitation: 7 Keys To A Successful Trial
The immunoprecipitation is an immunoassay often used which uses immobilized antibodies on a solid support to isolate, from a complex…
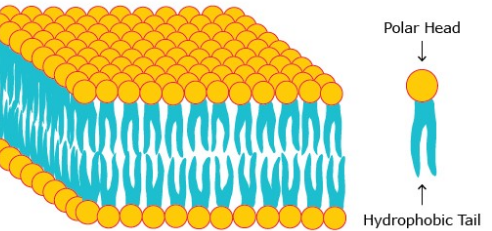
How To Remove Detergents In Protein Samples
The detergents are reagents mandatory within the processes of extraction, purification and / or protein solubilization within the…
Fish-Pak: Fish species dataset from Pakistan for visual features based classification.
Fishes are most various group of vertebrates with greater than 33000 species. These are recognized based…
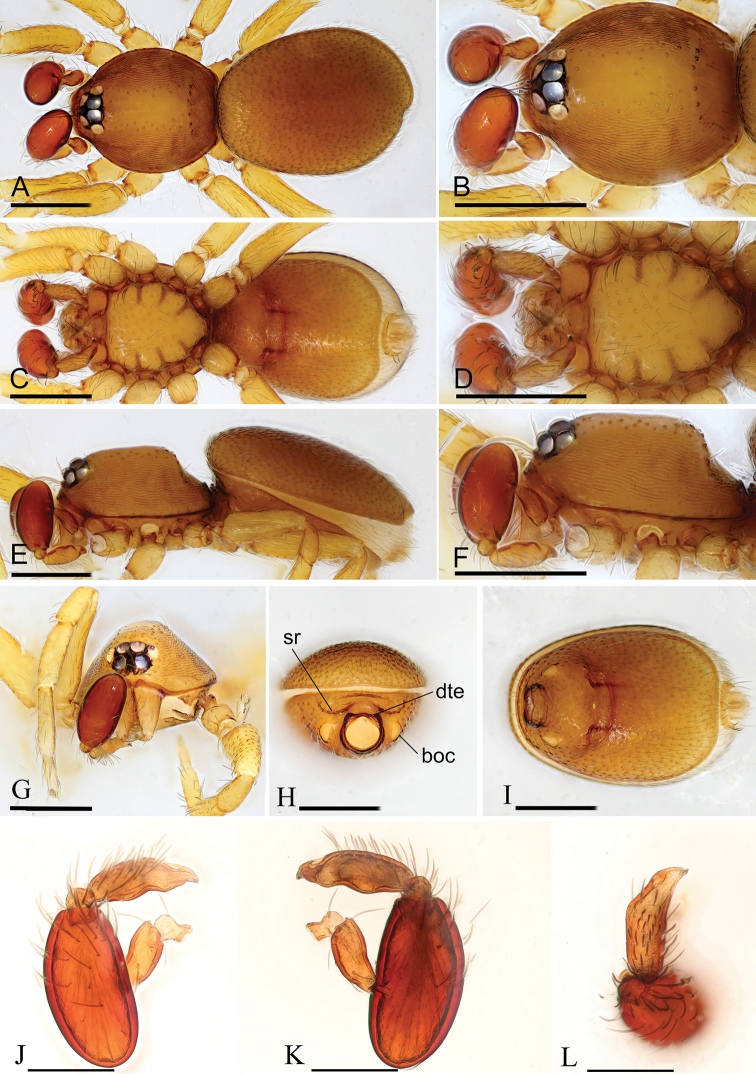
Two new species of the genus Opopaea (Araneae, Oonopidae) from Myanmar.
Two new species of the genus Opopaea Simon, 1892 are reported from Myanmar, O. kanpetlet Tong & Li, sp. nov. (♂♀) and O.…